Telemedicine Reaches Far and Wide
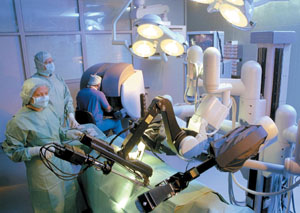 |
| A surgeon sitting at a console (rear) uses an Intuitive Surgical Inc. Da Vinci robotic surgical system to operate on a patient. The U.S. Army employs one of these robots and is experimenting with systems that would allow a doctor to operate tens of thousands of miles distant. |
Research plans a telerobotic future for medics and physicians.
On the battlefield of the future, a U.S. Army soldier is hit by shrapnel from an artillery round and is rendered unconscious with internal injuries to his torso. He is alone and no one witnesses his injury, but the intelligent agents in his automated self-monitoring system detect that he is in crisis, and the system transmits a signal to a regional command center. Officers at the command center dispatch an unmanned rescue vehicle, which enters the live-fire zone and deploys small robots to collect him carefully for removal from the hot zone.
The soldier receives emergency care on the unmanned rescue vehicle, where he is placed on a life-support trauma and transport platform. It provides oxygen and pain control as diagnosed by microelectromechanical sensors and automated systems. He is transported in this personal intensive care capsule—by unmanned helicopter, if necessary—to a surgical center established near the front, where he can receive medical attention quickly. By the time he arrives at the center, a computer has combined personal data from his metabolic monitoring chip with information from multiple automated diagnostic instruments that use noninvasive procedures to provide an accurate assessment of his life-threatening condition.
With this information in hand, a surgeon specializing in this soldier’s type of injuries swings into action. Based several hundred miles away, the surgeon directs on-the-scene experts trained in emergency medical response to position robotic surgical equipment. The surgeon fits her hands into special sensing brackets as the emergency personnel stabilize the patient to maintain his vital signs during the surgery. The surgeon then begins the operation by choosing from among several image perspectives from cameras placed at different positions around this combat operating room. As the doctor moves her hands, robotic instruments around the patient mimic her motions to perform emergency surgery on the stricken soldier. When a minimally invasive incision is made and robotic probes enter the patient, the doctor views the real-time internal imagery on a large screen in front of her. Simultaneously, she can view the patient’s diagnostic scans displayed directly on her retina as she proceeds with the surgery.
If the surgeon discovers an unforeseen situation, she can call up reference material for immediate display either through her eyeview or on a nearby display screen. If the original diagnosis was wrong and the new diagnosis will require a different area of specialty, she can hand off the surgery to a colleague at yet another location without even removing the robotic instruments from the patient. Whichever way events go, a successful surgery is followed by the patient being transported to a recovery facility with doctors monitoring his condition every step of the way—remotely, of course.
This scenario from the future battlefield is making its way into the force incrementally. U.S. Army medical experts are bringing telemedicine to the battlefield in steps that provide marked improvements in medical care with each advance. As these technologies are improved and complemented by other innovations, the ability of U.S. military medical personnel to treat battlefield injuries will increase inversely to the number of soldiers who die as a result of their wounds. And, many of these advances undoubtedly will find their way into public medicine.
Many innovations already have been implemented in Afghanistan and Iraq (see page 62), but researchers are pursuing technological breakthroughs that would render today’s state-of-the-art systems mundane in just a few years. Their efforts include a program known as the Operating Room of the Future, or ORF.
Ronald Marchessault Jr., senior project officer for the ORF program in the clinical applications division at the Telemedicine and Advanced Technology Research Center (TATRC), U.S. Army Medical Research and Materiel Command, Fort Detrick, Maryland, explains that the two-year-old program focuses on several medical research areas. Three of these cover advanced devices, medical informatics and telesurgery, and the others focus on disciplines that have crossover applications.
Some of these efforts are geared toward advancing the state of the art in surgery, while others aim toward a goal related to Army medical needs that also could be applied elsewhere. These range from improved patient information access to the use of unmanned air vehicles for providing telesurgery communications links.
Col. Ronald K. Poropatich, USA, senior clinical consultant to the TATRC and a medical doctor, relates that some aspects of this effort seek to improve tools and techniques that date back to before the Industrial Age. “We are doing 21st-century surgery on 15th-century platforms with 19th-century instruments,” he observes. “We’re trying to go beyond operating rooms as isolated worlds run by feudal lords with patients strapped to slabs, where the instruments are primitive, rigid, inflexible, ergonomically awkward and have limited tactile sense.”
Marchessault relates that the largest ORF effort focuses on advanced devices. Research into spinal injuries, for example, looks both at causes and surgical devices that can alleviate pain or enhance recovery. Another effort aims to empower a robot to assist a human surgeon during an operation by providing instruments and keeping track of inventory.
Changing the nature of these surgical instruments is part of the program. Robotic laser tissue welding would provide new ways of cauterizing wounds and repairing damaged tissue. A related thrust is to take ultrasound and focus it as an internal therapeutic tool. The TATRC’s high-intensity focused ultrasound program has three projects conducted with academia aiming at dual-use systems. Instead of being just a diagnostic tool, an ultrasound system would employ a transducer that would allow it to both detect an internal hemorrhage and cauterize it. The goal is to develop a system that does not need to even penetrate the skin.
An effort aimed at integrated technology for patient monitoring attempts to capture all of the information being provided in the operating room by doctors and devices. This would combine sensor readings with live actions to generate an overall picture of events that establishes strong links between causes and effects.
Dr. Gerald R. Moses, director of the clinical applications division at the TATRC, explains that all of these efforts will save lives in a variety of ways. “We will be getting to the casualty earlier; we will get there with more effective interventions; and the level of intervention will be better, more accurate and more focused on safety than any have been before.”
Medical imagery is a vital component of these future capabilities, both for surgeons in remote locations and for battlefield doctors or medics who may need to access imagery in a crisis situation. In an effort known as telesurgical mentoring, videoconferencing cameras placed in the lights above the operating table send images of the surgeon’s view to consultants in remote locations. This capability already is being used in Afghanistan, where general surgeons operating on a patient can consult with a neurosurgeon in Washington, D.C., via videoconferencing link.
The next step will be to enable the distant surgeon to perform the operation on a remote patient. This will be enabled by a surgical robot that performs the surgical duties based on input from the distant surgeon. The Army already has a commercially manufactured surgical robot made by Intuitive Surgical Inc., Sunnyvale, California, known as Da Vinci, in Walter Reed Army Hospital in Washington. Guided by a surgeon who sits at a console a few feet from the operating table, this robot performs surgery that includes extending an arm into the patient. The nearby surgeon views the operation in three-dimensional (3-D) vision through imagery supplied by the robot’s cameras.
Scientists already are demonstrating a prototype remote surgery imaging system, that includes special glasses to permit surgeons to view CAT scans or MRIs. These diagnostic images could be displayed on the doctor’s retina off to the side in a position that does not interfere with the doctor’s view of the surgery itself.
There are several reasons that a robot is used even when the appropriate surgeon is present. One is that the robot reduces fatigue on the surgeon who no longer must angle his or her arms awkwardly over—or into—the patient. The surgeon can assume a comfortable position while manipulating the robotic arms, and this will improve the doctor’s ability to perform the surgery without incident.
 |
| A prototype robotic medical rescue vehicle rolls out in a demonstration. In future combat, casualties may be treated and removed entirely from the battlefield by robotic vehicles and systems. |
Researchers are working to upgrade existing surgical robots to make them smaller, modular and more multifunctional. The modular approach would offer a host of new capabilities. A single robot would be able to perform neurosurgery as well as patient monitoring based on the modules attached to it.
Having a surgeon run a nearby robot configured to an operating room table is only an intermediate step, however. The ultimate goal remains to enable surgeons to perform telerobotic surgery thousands of miles away from the patient.
“If you can extend a specialist’s skill sets from the continental United States into distant remote locations, then you add a tremendous amount of value [to medical care],” Marchessault says. “And, if you can reduce the footprint of people on the battlefield through technology advances, then you save lives that way and improve the life expectancy of the patient.”
One of the biggest hurdles to overcome is signal latency. A surgeon connected via satellite links to an operating room on the other side of the globe will encounter a discernible time lag between his or her hand-guided robot commands and the robot’s actual movements as the doctor views them on a display. The farther the surgeon is based from the patient, the greater the problem of latency, Col. Poropatich states. At a great enough distance, the latency becomes unacceptable.
In 2001, doctors in the United States conducted a trans-Atlantic telerobotic gall-bladder operation on a patient in France. This required more than $150 million in telecommunications investment for 8-megabit-per-second connectivity between New York and Strasbourg to mitigate the latency problem. The round-trip delay was 155 milliseconds.
Moses relates that researchers have discovered how to reduce latency by making adjustments in the transmission system. Scientists are working on devices and technology issues that would address the amount of latency. Also, research has determined that surgeons can tolerate some latency. Col. Poropatich notes that the top threshold for surgery is a latency of about 330 milliseconds.
In areas lacking a fiber infrastructure, unmanned aerial vehicles could provide high-capacity linkage—greater than 50 megabits per second—with a latency of less than 1 millisecond.
Achieving the goal of effective robotic surgery will require advances in miniaturization, articulating handheld instruments, robotics and 3-D vision. Early robot surgical devices were little more than chopsticks, Col. Poropatich relates. Researchers want surgical robots to have instruments with freedom of motion that mimic human hands. New imaging systems provide 3-D views with as much as 15X magnification and enhanced resolution, depth and contrast.
In addition to mechanical engineering challenges, researchers must develop materials that are lighter and less bulky, yet strong and efficient, Moses concedes. The technology that makes this possible does not exist yet, he adds.
Above all, Col. Poropatich notes, it comes down to the computer interface between the surgeon and the patient. The goal is for robots to enhance human visualization, strength, precision and degrees of motion—and to extend the surgeon’s reach far beyond the hospital.
For telerobotic surgery, the additional challenges involve telecommunications connectivity, bandwidth and compression algorithms. And, the speed of light becomes a limiting factor with satellite connectivity over tens of thousands of miles.
“There is a degree of intervention that we anticipate being done telesurgically while the patient is in transit to a higher level facility—or even while the casualty is awaiting safe extraction,” Moses offers. “We also envision a time in the future when causalities will be recovered and stabilized robotically.”
Amid this sea of information technologies, modeling and simulation plays a key role. Marchessault explains that doctors can improve psychomotor skills and practice risky clinical procedures using medical simulators. The TATRC has a significant group of more than 80 projects representing more than $60 million of research investment, he allows.
Some of these simulations give the medical personnel the actual feel of a procedure. Marchessault cites one that simulates the insertion of a chest trauma tube. A mannequin-based simulator supported by a personal computer replicates the visual, haptic and medical experience of putting a chest tube into a human body, he reports. Another existing simulation reproduces the creation of an emergency airway in a life-saving situation.
These simulations focus on training medical personnel in a controlled environment. However, the effort also is progressing to where simulations could instruct emergency responders in the field. This thrust has a way to go, Marchessault allows, but it is a goal. In effect, it could take the form of a digital medical manual in the same manner that vehicle maintenance manuals have been digitized.
For medical conditions that do not require immediate emergency action, researchers are looking at virtual surgery to permit simulating a specific robotic operation before the actual procedure is undertaken. This would involve 3-D imagery construction and 3-D instrument positioning. Doctors would collaborate to determine the plan that would produce the best surgical outcome and then a robot could be programmed to achieve that outcome.
In this scenario, a soldier’s diagnostic scan would be sent back from the battlefield to specialists in the United States who would integrate that scan into an algorithm connected to a telesurgical capability. This program would help determine how to treat the patient, and the doctors then would add the individual’s body dimensions to program the robot to perform that surgery.
Dog Tags Join Wireless Revolution The entire menu of these telemedicine advances may not be ready for another 15 to 20 years, U.S. Army officials say. However, some aspects are about to be added to the Army medical kit. Soldiers currently have an information dog tag that contains vital medical history data. The Army’s Battlefield Medical Information System for Telemedicine, or BMIST, is a handheld personal digital assistant that allows medical personnel to store, retrieve or transmit data from these dog tags and from individual treatments. This handheld point-of-care device also can help medical personnel treat sick or wounded soldiers, and its next iteration may make it more interactive with the soldier. Currently, the electronic dog tag is inserted into the BMIST unit to be accessed by the health professional. This year, the Army will test a prototype that would give the information dog tag the ability to talk to the BMIST unit from as far away as 6 feet. This capability eliminates the need for the dog tag to be placed within the handheld unit. |
Web Resources
U.S. Army Telemedicine and Advanced Technology Research Center: www.tatrc.org
U.S. Army Medical Research and Materiel Command: https://mrmc.detrick.army.mil
Intuitive Surgical Inc.: www.intuitivesurgical.com




Comments